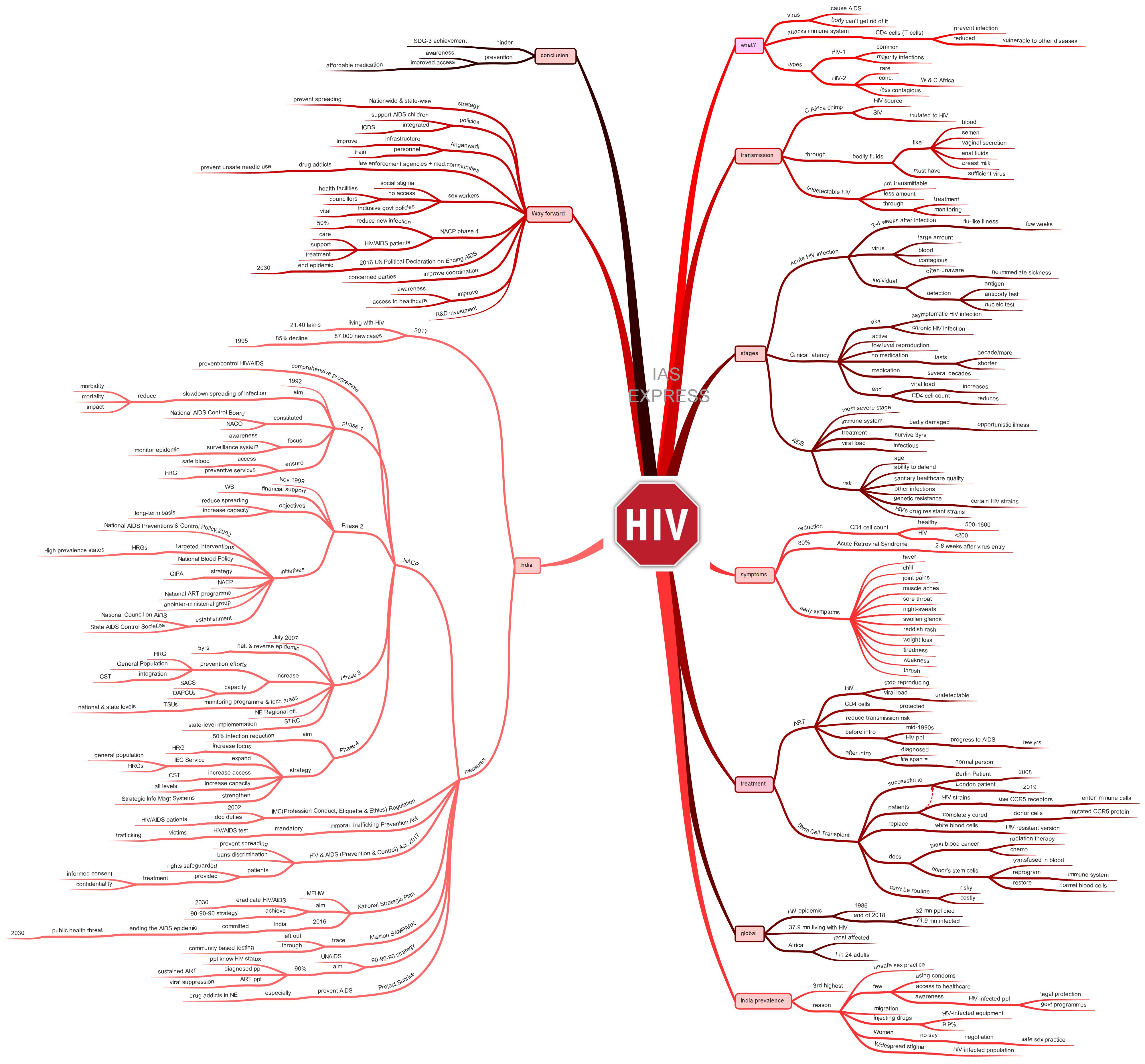
HIV/AIDS in India: The Road to Eradication

This year, an individual (London Patient) was treated in London and was completely cured of HIV. CCR5-delta 32 technique, based on stem cell transplant involving the use of CCR5-delta 32 homozygous donor cells, was used to cure him. This is significant progress as only two individuals have currently been cured of HIV.
What is HIV?
- HIV or Human Immunodeficiency Virus is a virus that can lead to Acquired Immunodeficiency Syndrome (AIDS) if not treated.
- Unlike many viruses, the human body cannot get rid of HIV completely in spite of the treatment.
- It attacks the immune system, specifically the CD4 cells (T cells), that help the immune system ward off infections.
- If not treated, HIV reduces the number of CD4 cells (T cells) in the body, making the individual more likely to get other infections and diseases.
- There are two types of HIV – HIV-1 and HIV-2
- HIV-1 is considered as the common type, representing a vast majority of infections globally. HIV-2 is rare and mostly concentrated in the West and Central African regions.
- While both of these types can lead to AIDS, HIV-2 is far more difficult to be transmitted and less contagious.
How is it transmitted?
- Scientists have identified a type of chimpanzee in Central Africa as the source for HIV. It is believed that the Chimpanzee version of the immunodeficiency virus (Simian Immunodeficiency Virus (SIV)) most likely to have transmitted to humans and mutated into HIV.
- It is transmitted from one individual to another through bodily fluids like blood, semen, vaginal secretion, anal fluids and breast milk.
- For HIV to be transmitted, the bodily fluids must have sufficient virus. The individual with “undetectable HIV” cannot transfer HIV to another individual even if the bodily fluid is transmitted.
- Undetectable HIV is the condition wherein the amount of HIV is so low that the blood test cannot detect it. Treatment with constant monitoring can provide for this condition.
What are the stages of HIV?
There are three stages of HIV infection. They are as follows:
Stage 1: Acute HIV Infection
- Within 2 to 4 weeks after the HIV infection, the individual may experience a flu-like illness, which may last for a few weeks.
- During this stage, there will a large amount of virus in the blood and is very contagious.
- However, the individual is often not aware of the infection because he/she does not feel sick right away or at all.
- To know whether someone has an acute infection, either an antigen or antibody test or a nucleic acid test is necessary.
Stage 2: Clinical latency
- This period is sometimes known as asymptomatic HIV infection or chronic HIV infection.
- During this phase, HIV is still active but reproduce at very low levels.
- There will be no symptoms or sickness during this period.
- If the affected individual is not taking medication to treat HIV, this period can last for a decade or longer, but some may progress through this phase faster
- The people who are medicated may be in this stage for several decades.
- At the end of this phase, the individual’s viral load starts to go up and the CD4 cell count begins to go down.
Stage 3: AIDS
- This is the most severe stage of HIV infection.
- The people with AIDS have such badly damaged immune systems that they get an increasing number of severe illnesses called opportunistic illness.
- With treatment, people with AIDS can typically survive for about 3 years.
- AIDS patients can have a high viral load and can be very infectious.
- The risk of progressing to this stage varies based on the individual and is highly dependent on:
- Individual’s age
- The ability of the body to defend against HIV
- The quality of sanitary healthcare
- Incidence of other infections
- The person’s genetic resistance to certain strains of the HIV
- Drug-resistant strains of HIV
What are the symptoms?
- The most common symptom of HIV infection is the reduction in the CD4 cell count. In a healthy body, the CD4 cell count is between 500 and 1600. In an HIV infected body, is can be less than 200.
- The weakened immune system would mean that the HIV-infected individual is highly prone to opportunistic infections and cancer. Recovery from even minor injury or sickness is difficult.
- Around 80% of the HIV-infected people would develop a set of symptoms known as Acute Retroviral Syndrome in around 2 to 6 weeks after the virus enters into the body.
- The early symptoms include fever, chill, joint pains, muscle aches, sore throat, night sweats, swollen glands, red rash, tiredness, weakness, unintentional weight loss and thrush.
How can it be treated?
Currently, there is no effective treatment for HIV. However, with proper medical care, HIV can be controlled.
Antiretroviral Therapy (ART):
- It is the medication used to stop HIV from reproducing.
- If the individual takes ART as prescribed, their viral load can become undetectable and CD4 cells will be protected to a certain extent.
- If the HIV stays undetectable, the infected individuals can live long, healthy lives and have effectively no risk of transmitting HIV to others.
- Before the introduction of ART in the mid-1990s, the people with HIV infection could progress to AIDS in just a few years.
- Today, someone diagnosed with HIV and treated before the disease is far advanced can live nearly as long as someone who does not have HIV.
Stem Cell Transplant:
- Timothy Brown “Berlin Patient” (2008) and “London Patient” (March 2019) are the only two HIV-infected individuals to have been completely “cured” of HIV.
- In this treatment, the HIV-infected individual is treated with stem cell transplantation, the one that involves the replacement of white blood cells with an HIV-resistant version.
- This procedure allows the doctors to blast blood cancer in the bone marrow with large doses of radiation therapy or chemotherapy.
- A donor’s stem cells are then transfused into the patient’s blood to reprogram the immune system and restore normal blood cell production.
- In the case of the above-mentioned patients, the donor cells used had a rare mutation of the CCR5 protein.
- Most HIV strains use CCR5 receptors to enter the immune cells in the body. If the transplanted cells are mutated and resist HIV, the virus cannot enter.
- This treatment, however, cannot be adopted as a routine treatment as the procedure is dangerous, costly and can be used only as a last resort.
Global status:
- The HIV epidemic started in 1986. Since then, 32 million people have died from AIDS-related diseases by the end of 2018.
- By the end of 2018, HIV has infected 74.9 million people since the start of the epidemic.
- Globally, 37.9 million people are living with HIV.
- Africa is the most affected by HIV at the global scale where 1 in 24 adults are living with HIV
India:
- The total number of people living with HIV was estimated to be 21.40 lakhs in 2017.
- India witnessed over 87,000 new cases in 2017 and saw a decline of 85% compared to 1995.
What are the measures taken by the government?
National AIDS Control Program (NACP)
- NACP is globally acclaimed as a success story. It was launched in 1992 as a comprehensive programme for the prevention and control of HIV/AIDS in India.
- Consequently, the focus has shifted from raising awareness to behaviour change, from national response to a more decentralised response and inclusion of the assistance from the NGOs and the involvement of networks of People Living with HIV/AIDS (PLHIV).
- As of now, the government has undertaken four phases of this programme:
- NACP I: Its aim was to slow down the spread of HIV infections to reduce morbidity, mortality and impact of AIDS in the country. National AIDS Control Board was set up and an autonomous National AIDS Control Organisation (NACO) was established to implement the initiative. In this phase, more focus was given to the awareness generation, setting up a surveillance system for monitoring the HIV epidemic, measures to ensure access to safe blood and preventive services for high-risk group populations.
- NACP II: It was launched in November 1999 with financial support from the World Bank. The policy and strategy shifted to focus on the following objectives:
- Reduce the spread of HIV infection in India
- Increase India’s capacity to respond to HIV/AIDS on the long-term basis.
The key initiatives taken by the government during this phase include:
- National AIDS Preventions and Control Policy,2002
- Increasing the Targeted Interventions for High-risk groups in high prevalence states
- Adoption of National Blood Policy
- Strategy for Greater Involvement of People with HIV/AIDS (GIPA)
- Launch of National Adolescent Education Programme (NAEP) and National ART programme
- Formation of the anointer-ministerial group for mainstreaming
- Establishment of National Council on AIDS, chaired by the Prime Minister and State AIDS Control Societies in all states.
- NACP III: It was launched in July 2007 with an aim to halt and reverse the epidemic within the 5-year project period by increasing the prevention efforts among the High-Risk Groups (HRG) and General Population and integrating them with Care, Support and Treatment (CST) services. Capacities of the State AIDS Control Societies (SACS) and District AIDS Prevention and Control Units (DAPCUs) have been strengthened. Technical Support Units (TSUs) were established at the national and state level to assist in the monitoring of the programme and technical areas. A North-East regional office was established for the special focus of the North-East states. State Training Resource Centres (STRC) was established as state-level implementation units and functionaries.
- Phase IV: Its objective include the reduction of infection by 50% and provide comprehensive care and support to the infected individuals. The strategies implemented in this phase include:
- Prevention through increased focus on high-risk groups (HRGs), vulnerable population and the general population
- Expanding Information, Education and Communication (IEC) service to the general population and HRGs.
- Increasing access and promoting comprehensive Care, Support and Treatment (CST)
- Building capacities at national, state, district and facility levels
- Strengthening Strategic Information Management Systems
Indian Medical Council (Profession Conduct, Etiquette and Ethics) Regulation, 2002
- It specifies the duties of the doctors towards the HIV/AIDS patients
Immoral Trafficking Prevention Act:
- It calls for a mandatory medical examination for the detection of HIV/AIDS among the victims of trafficking.
HIV and AIDS (Prevention and Control) Act, 2017:
- It aims to prevent the spread of HIV/AIDS
- It bans discrimination against the HIV/AIDS-infected individuals
- As per the Act, it is the duty of the establishments to safeguard the rights of the patients affected by HIV/AIDS and provide for informed consent and confidentiality concerning the treatment.
National Strategic Plan:
- Launched by the Union Ministry of Health and Family Welfare, its aim is to eradicate HIV/AIDS by 2030.
- In 2016, India, in the UN’s High-Level Meeting on AIDS, had committed towards the goal of “ending the AIDS epidemic as a public health threat by 2030”.
- This strategy may pave the way for the achievement of the 90-90-90 strategy.
Mission SAMPARK:
- It aims to trace those who are left to follow up. These individuals are brought under the ART services.
- This community-based testing will enable the identification of all those who are HIV positive.
90-90-90 strategy:
- It is a UNAIDS programme that has the following targets:
- 90% of all people living with HIV will know their HIV status
- 90% of all people with diagnosed HIV infection will receive a sustained antiretroviral therapy
- 90% of all people receiving ART will have viral suppression
Project Sunrise:
- It aims to prevent AIDS, especially among drug addicts in North East India.
What is the reason for the prevalence of HIV in India?
India has the third-largest HIV/AIDS infected population. The following are the reasons behind this situation:
- Unsafe sex practice
- Only a few are making use of condom
- Migration of the population
- Injecting drugs using HIV-contaminated equipment. It has caused the 9.9% of the HIV cases.
- Women having limited to no say on negotiation for safer sex practice
- Widespread stigma towards HIV-infected people despite the government measures. The marginalised are especially vulnerable, leading to them having limited to no access to medical treatment.
- Limited access to the healthcare system
- There is only limited awareness about the legal protection and government aids to the HIV-infected people.
What can be the way forward?
- A comprehensive nationwide and state-wise strategy to prevent the spread of new HIV infections must be planned and enforced.
- Innovative policies must be executed for AIDS-infected children by integrating them with the Integrated Child Development Services (ICDS).
- Anganwadi infrastructures must be improved to support these children and faculties working in these facilities must be provided with special training to prevent the spread of infection.
- Law enforcement agencies and the Police must coordinate with the medical community to ensure the drug addicts are not indulging in unsafe use of needles.
- Sex workers always face stigma in society, leading to them not having access to health facilities, councillors etc. Inclusive government policies must be implemented to address this issue.
- National AIDS Control Programme (NACP) Phase IV aims to diminish the new infections by 50% and provide comprehensive care, support and treatment to all those who are infected by AIDS/HIV.
- The objective of the 2016 UN Political Declaration on Ending AIDS is to end the epidemic by 2030.
- The government must ensure the target is achieved through improved coordination with the concerned parties and also execute new policies to improve healthcare facilities and awareness related to AIDS.
- Increased investment in research and development can further improve the situation.
Conclusion
HIV is one of the major hindrances when it comes to achieving the Sustainable Development Goal 3 – Ensuring healthy lives and promoting wellbeing for all at all ages. This is because there is no efficient treatment to deal with this disease. Thus, prevention through awareness and improved access to affordable medication is a necessary step that all governments should undertake to deal with this issue.
Test yourself
What is HIV? What can be done to prevent the spread of this disease?
If you like this post, please share your feedback in the comments section below so that we will upload more posts like this.