Epidemic Diseases Act, 1897: Origin, Importance & Limitations

On March 11, 2020, the Cabinet Secretary announced that all states and UTs should invoke provisions of Section 2 of the Epidemic Diseases Act, 1897 so that Health Ministry advisories are enforceable. As the number of cases in India has crossed 120 and is already in Stage 2 (local transition) of COVID-19, it is vital to enforce necessary measures to prevent the country from moving to stage 3, which involves community transmission of the disease. The Epidemic Diseases Act, despite being more than 100 years old, is playing a crucial role in dealing with the current outbreak. However, this colonial-era law has numerous limitations that need to be reformed to prepare the country of future epidemic outbreaks.
This topic of “Epidemic Diseases Act, 1897: Origin, Importance & Limitations” is important from the perspective of the UPSC IAS Examination, which falls under General Studies Portion.
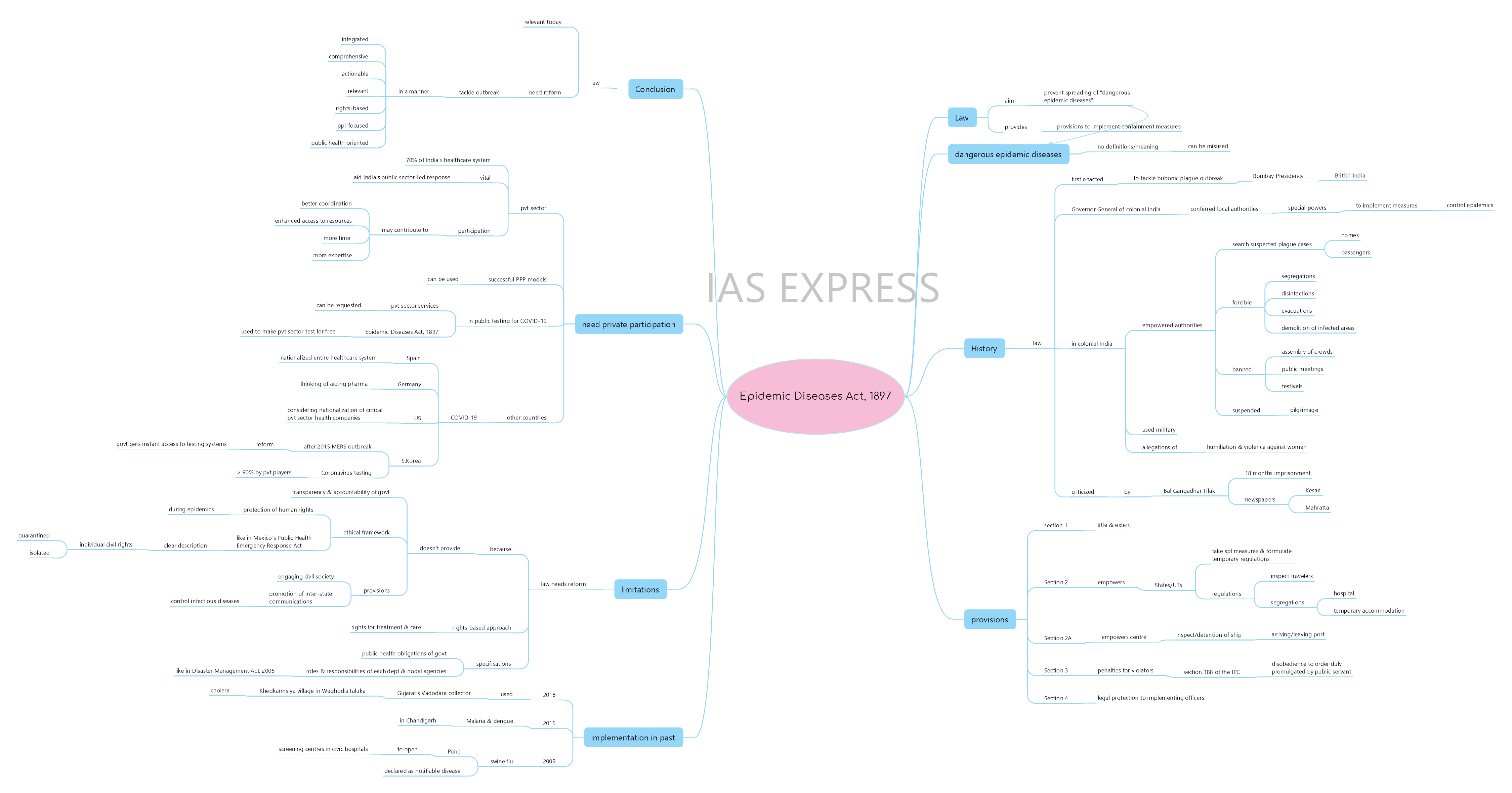
What is the Epidemic Diseases Act, 1897?
- The colonial-era Epidemic Disease Act, 1897 is a law that was routinely enforced across the country to deal with outbreaks of diseases like swine flu, dengue, and cholera.
- This law provides special provisions that are required to implement containment measures to control the spread of the disease.
- This Act aims to prevent the spread of “dangerous epidemic diseases”.
What is “dangerous epidemic diseases” under this Act?
- Epidemic Diseases Act, 1897 does not provide any definition or description for the term “dangerous epidemic diseases”.
- There is no clear definition of whether an epidemic is “dangerous” based on the magnitude of the problem, the severity of the problem, the age of the population affected or it’s potential to spread internationally.
- Thus, due to the lack of such details, it can be easily misused.
How did this law come to be?
- The Epidemic Diseases Act, 1897 was first enacted to tackle the spread of bubonic plague in the erstwhile Bombay Presidency in British India.
- The Governor-General of colonial India conferred the local authorities with special powers to enable them to implement necessary measures to control the epidemic.
- In 1897, the year when this Act was enforced, Bal Gangadhar Tilak was imprisoned for 18 months after his newspapers Kesari and Mahratta criticised the imperial authorities for their handling of the plague epidemic.
- During the time the enactment, this law was vigorously enforced to control the plague epidemic.
- The powers it conferred were invoked to search suspected plague cases in homes and among passengers.
- There were forcible segregations of affected persons, disinfections, evacuations and demolition of infected places.
- Assembly of crowds, public meetings and festivals were banned and pilgrimages were suspended.
- During this time, there were allegations of humiliation and violence against women due to this law, leading to the breaking of riots.
- In many places, the military was used by the colonial government to implement this law.
- Since independence in 1947, this colonial-era law continues to find relevance in tackling epidemics and has been used by the Indian government several times to successfully restrain the outbreak of diseases.
What are the provisions of the Epidemic Diseases Act, 1897?
- It is one of the shortest Acts in India, comprising of just four sections.
- The first section explains the title and the extent.
- Section 2 gives powers to the state/UTs to take special measures and formulate regulations to contain the spread of disease.
- This section states that when a state government is satisfied that the state or any part thereof, is threatened with a dangerous epidemic disease outbreak, the state government if it thinks that ordinary provisions of the law are insufficient, it may take necessary measures and prescribe temporary regulations that are to be observed by the public.
- The state government may also take measures and prescribe regulations for the inspection of persons travelling by railway or otherwise, and segregation, in hospital, temporary accommodation or otherwise, of persons suspected by the inspecting officer of being infected by any such disease
- Section 2A empowers the Central Government to inspect any ship leaving or arriving at any port and for detention thereof, or of any person intending to sail therein, or arriving thereby.
- Section 3 describes penalties for violating the regulations, under section 188 of the IPC (disobedience to order duly promulgated by public servant).
- Section 4 deals with legal protection to the implementing officers acting under the Act.
How was it implemented in the recent past?
- In 2018, the district collector of Gujarat’s Vadodara issued a notification under the Act declaring the Khedkarmsiya village in Waghodia taluka as cholera-affected.
- The Act was implemented in 2015 to deal with malaria and dengue outbreak in Chandigarh. Controlling officers were instructed to ensure the issuance of notices and challans of Rs.500 to all offenders.
- In 2009, Section 2 was invoked to tackle swine flu outbreak in Pune to open screening centres in civic hospitals across the city, and swine flu was declared a notifiable disease.
What can the limitations of the law?
- The Epidemic Diseases Act, 1897 has numerous limitations, as it does not explain many ambiguous terms within its provisions, nor provides due procedures that are to be taken during the times of crisis.
- It does not provide for accountability and transparency of the government.
- This law requires changes based on a rights-based approach that upholds the right to treatment and care.
- Changes are also required so that the Act specifies the public health obligations of the government.
- For better accountability, the law should specify the roles and responsibilities of each department and nodal agencies for the prevention and control of epidemics.
- For instance, the Disaster Management Act, 2005 describes in detail when to act, who should act, what measures are to be taken at different levels, how to implement, how to coordinate, and what the roles and responsibilities of each department and authorities during the emergencies.
- This law does not provide an ethical framework or protection of human rights during the response to the epidemic. This necessary as during the times of emergency, there may be little to no consideration for ethics.
- For instance, the Public Health Emergency Response Act in Mexico provides a clear description of individual civil rights of persons quarantined or isolated.
- Also, provisions for engaging and strengthening the civil society and measures for promoting inter-state communications for the control of infectious diseases should be considered under the legal framework.
Why should the private health sector need to contribute during epidemics?
- The private sector accounts for nearly 70% of India’s healthcare, this sector has a critical role to play in assisting the traditional public sector-led response to the prevention and tackling of outbreaks.
- There are many successful public-private partnership (PPP) models in healthcare that can be used for better participation of the private sector during the epidemic outbreak.
- Investing in mechanisms to bring private players may contribute to better coordination, enhanced access to resources, more time and expertise during epidemics. Providing mechanisms to ensure these are a need of the hour.
- Recently, the World Health Organisation had laid great emphasis on testing for all suspected Coronavirus cases.
- However, a country as large and populous as India, the government does not have the necessary resources to undertake mass testing all by itself.
- Currently, India has more than 50 labs for testing. However, this is insufficient for a country with more than 1.3 billion people.
- Necessary measures must be taken to include private health sector while tackling this outbreak.
- For instance, Spain, having only a fraction of India’s size and population, has decided to take over private health care services. The entire Spanish healthcare system has been nationalised.
- Other countries too are considering different forms of nationalisation.
- Germany is thinking about aiding pharmaceutical companies.
- The USA is considering to take over critical private-sector health companies
- South Korea had increased its testing capabilities by involving the private sector, leading to a reduction in the number of positive cases. After the MERS outbreak in 2015, the country enacted a key reform that allowed the government to almost an instantaneous approval to gain access to testing systems. For the coronavirus testing, more than 90% of the testing is done by private players.
- India could adopt similar strategies in its fight against the coronavirus outbreak.
- Services of the private sector could be requisitioned.
- Nationalization seems to be the only way to deal with the shortages and to ensure that all people get the required treatment
- The Epidemic Diseases Act, 1897 can be used to involve private sector participation while tackling this epidemic.
Conclusion:
The Epidemic Diseases Act, 1897, which is more than a century old, still finds relevance today as it constantly helps prevent and control entry and spread of communicable diseases in India. The century-old law, as it is vital in the present-day context, must be reformed so that there is an integrated, comprehensive, actionable and relevant legal provision for controlling outbreaks in India that is enunciated in a rights-based, people-focused and public health-oriented manner.
Practice Question for mains:
What is the Epidemic Diseases Act, 1897 that was recently enforced to tackle the COVID-19 outbreak? Discuss how it can be used to deal with the epidemic.