Significance of Cervavac
This topic of “Significance of Cervavac” is important from the perspective of the UPSC IAS Examination, which falls under General Studies Portion.
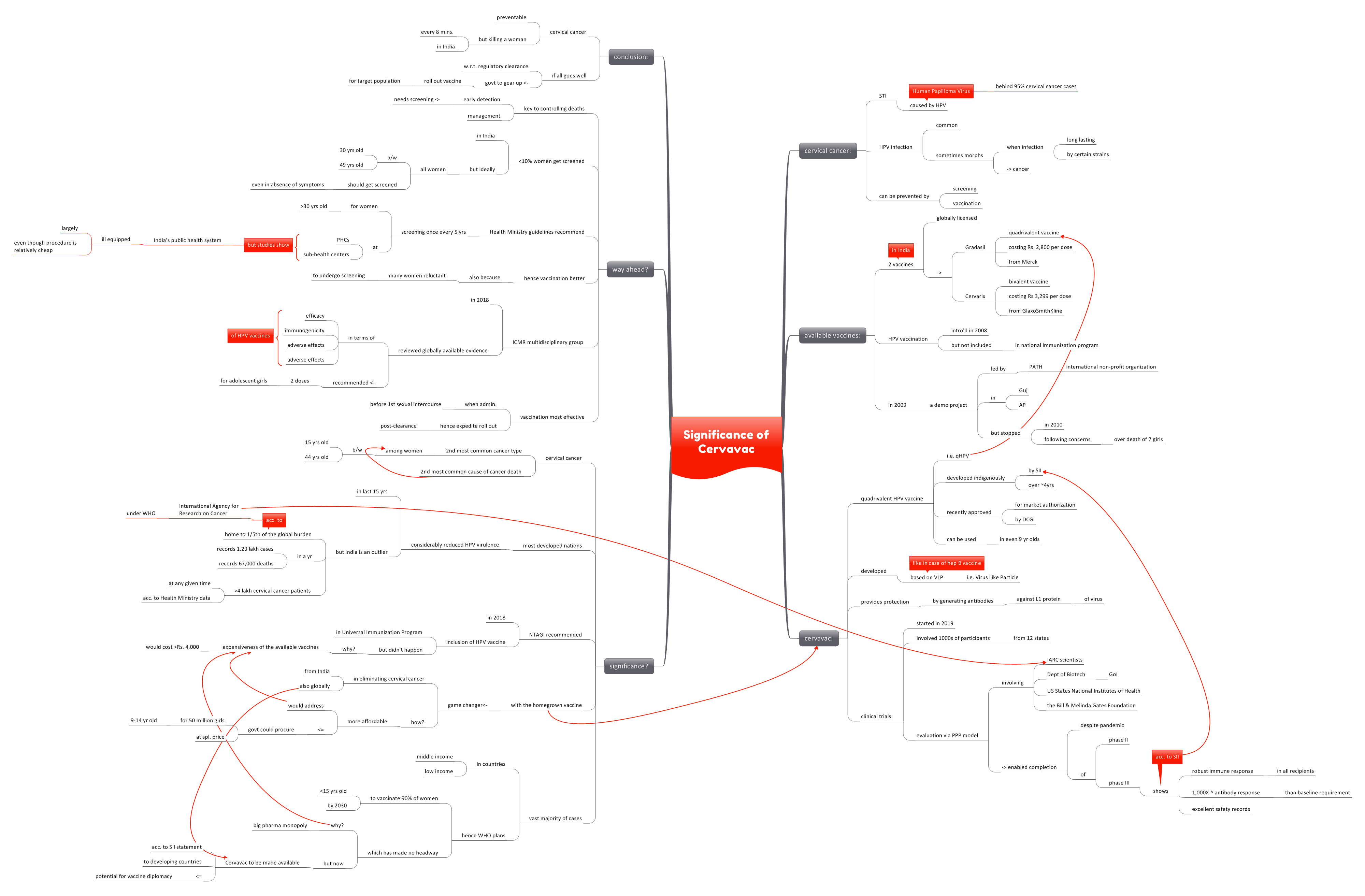
What is Cervical Cancer?
- Cervical cancer is a sexually transmitted disease, caused by the HPV or Human Papilloma Virus. HPV is responsible for over 95% of cervical cancer cases.
- Though HPV infection is common, long-lasting infection by certain strains of HPV translate into cancer in the host.
- Currently, cervical cancer is prevented through screening and vaccination.
What are the available vaccines?
- Currently, 2 globally licensed vaccines are available in the country:
-
- Gradasil– a quadrivalent vaccine, costing Rs. 2,800 per dose, from Merck
- Cervarix– a bivalent vaccine, costing Rs 3,299 per dose, from GlaxoSmithKline
- HPV vaccination was introduced as early as 2008. However, it is yet to be included in the national immunization program.
- In 2009, a vaccine delivery and demonstration project was started in Gujarat and Andhra Pradesh. This project was led by PATH, an international non-profit organization. However, following reports of death of 7 girls who had received the vaccine, the project was suspended in 2010.
What is Cervavac?
- Cervavac is the country’s 1st quadrivalent HPV vaccine (qHPV).
- It was developed indigenously by Serum Institute of India. This vaccine has been in the making for nearly 4 years.
- It recently received approval for market authorization from the DCGI (Drug Controller General of India).
- This vaccine can be used in individuals as young as 9 years old.
- It was developed based on VLP or virus like particles, similar to hep-B vaccine (for hepatitis).
- It provides protection against the disease by generating antibodies against the virus’ L1 protein.
- Clinical trial for the vaccine started in 2019 and involved thousands of participants from 12 states.
- The vaccine was evaluated in a PPP model (public-private partnership)- involving IARC scientists, Indian Government’s Department of Biotechnology, US States National Institutes of Health and the Bill & Melinda Gates Foundation. This model enabled the completion of phase II and III trials, despite the pandemic.
- According to SII, phase III trials showed robust immune response in all the recipients. The vaccine’s antibody response is reported to be 1,000 times more than the required baseline, against all types of HPV. The results also showed excellent safety records.
Why is it significant?
- Cervical cancer is the 2nd most common cancer type among women between 15 and 44 years. It is also the 2nd most common cause of cancer death among this category of women.
- Most of the developed nations have considerably reduced HPV virulence in the last 15 years. However, India remains an outlier.
- India is home to 1/5th of the global burden of cervical cancers according to International Agency for Research on Cancer, under WHO. In a year, the country records 1.23 lakh cases and some 67,000 deaths.
- According to Health Ministry data, there are over 4 lakh cervical cancer patients at any given time, in India.
- In 2018, the NTAGI (National Technical Advisory Group on Immunization) recommended the inclusion of HPV vaccine in the Universal Immunization Program. However, the expensiveness of the available vaccines proved a deterrent i.e. the regimen would cost above Rs. 4,000.
- Now, with the DCGI’s approval, the homegrown vaccine could be a game-changer in the fight against cervical cancer.
- Cervavac is likely to be available at a more affordable cost than the currently available vaccines.
- With the approval, the government will be able to procure sufficient HPV vaccines for some 50 million girls in the 9-14 years age group. The vaccines might be procured at a special price.
- This would be a huge step in accelerating cervical cancer elimination, not only from India, but globally- according to a statement from IARC-WHO.
- A vast majority of these deaths occur in middle- and low-income countries. WHO has been planning to vaccinate 90% of women under 15 years by 2030. However, the plan hasn’t seen any progress- mainly because of the big pharmaceutical companies’ monopoly on HPV vaccines.
- SII stated that Cervavac is to be made available to developing countries in the ‘near future’. Hence, there is a huge potential for India, with regards to vaccine diplomacy.
What is the way ahead?
- Early detection and management are key to controlling cervical cancer deaths.
- Less than 10% of women get screened for cervical cancer in India. Ideally, all women, between 30 and 49 years of age, must get screened- even in the absence of symptoms.
- The Health Ministry guidelines call for screening every 5 years, for women over the age of 30 years. This screening can be undertaken at primary health centers and sub-health centers. However, studies show that India’s public health system is still largely ill-equipped to carry out such gynaecological procedures- even though they are relatively inexpensive.
- Hence, vaccination is a better option, also because it is difficult to convince many women to undergo screening process.
- In 2016, an ICMR multidisciplinary group looked into the globally available evidence of efficacy, immunogenicity, adverse effects and economics of HPV vaccines. The group recommended the administration of 2 doses to adolescent girls.
- As vaccination is most effective when administered before an individual’s 1st sexual intercourse, efforts must be made to expedite the new vaccine’s deployment, post-clearance from the regulators.
Conclusion:
Cervical cancer, despite being a preventable disease, kills a woman every 8 minutes in India. If all goes well with the regulatory clearance, the government must gear up to roll out the vaccine for the target population.
Practice Question for Mains
What is Cervavac? Examine the significance of its development. (250 words)