Oxygen Crisis in India

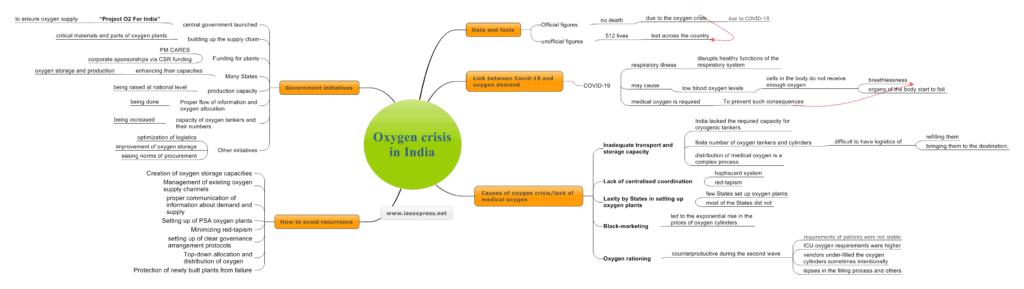
The COVID-19 pandemic has shaken the very dynamics of the global health infrastructure. Countries like India have been the worst sufferers. India, where the first wave of the pandemic could not wreak as much havoc as it did in some other countries, the second wave showed that it still has a lot to do to improve its health and essential medical supplies infrastructure. Of many reasons why the second wave of the pandemic could be called more deadly in India, one of the major ones is the oxygen crisis in India. The oxygen crisis devastated people’s lives and exposed the bleak state of the public health system in India. Thus, what becomes important is to know the reasons behind such a crisis and how India can avoid it in the coming time when the third wave is knocking at the door.
This topic of “Oxygen Crisis in India” is important from the perspective of the UPSC IAS Examination, which falls under General Studies Portion.
Data and facts
- Although official figures indicate that there was no death in India due to the oxygen crisis, the unofficial figures have estimated that as many as 512 lives were lost across the country due to oxygen shortage or denial.
- The crisis began to be noticed during the peak of the first wave in September 2020, and recurred with a greater magnitude during the peak of the second wave, in April and May 2021.
- The sudden rise in demand noticed across the country was from 3,842 MT per day on 12 April 2021 to 8,400 MT per day by 25 April, and further up to 11,000 MT per day by the beginning of May—before gradually reducing as the number of fresh COVID-19 cases declined.
- It was reported that to cater to the rising demands, India lacked resources as it only had around 1,200 cryogenic oxygen tankers across the country which was insufficient for servicing the surging requirements.
- In India, since the pandemic has taken over, both hospitals that treat COVID-19, and those that do not, suffered a shortage of medical oxygen.
What is the link between COVID-19 and oxygen demand?
- COVID-19, being a respiratory illness, disrupts healthy functions of the respiratory system and may cause low blood oxygen levels at some point in time.
- When oxygen levels in the body deplete due to COVID-19 infection, the cells in the body do not receive enough oxygen to perform normal bodily functions.
- Given that the oxygen levels continue to remain low, patients face breathlessness and different parts and organs of the body start to fail and collapse which may be fatal.
- To prevent such consequences, medical oxygen is required as without it patients may suffocate and die.
What was/were the cause/causes of the lack of medical oxygen/oxygen crisis in India?
- Inadequate transport and storage capacity
- India has a lack of enough transport and storage capacity. Liquid oxygen at very low temperatures requires to be transported in cryogenic tankers to distributors, which then convert it into gas for filling cylinders. But India lacked the required capacity for cryogenic tankers.
- Similarly, given the finite number of oxygen tankers and cylinders around, it was difficult to have logistics of refilling them and bringing them to the destination.
- Furthermore, the distribution of medical oxygen is a complex process.
- Large hospitals are usually supplied directly by manufacturers that use tankers to transport the oxygen.
- Whereas medium and small hospitals, as well as nursing homes, depend primarily on intermediaries. The manufacturers supply liquid oxygen to filling stations, again via tankers; gas agencies, who own cylinders, then get them filled in filling stations and thereafter supply them to the nursing homes.
- This entire supply chain was severely disrupted at multiple levels due to the steep and sudden rise in demand across the country.
- Lack of centralised coordination – Although India managed to deal with the oxygen crisis in some States during the first wave of the pandemic, the lack of centralised coordination in transporting oxygen from oxygen-abundant to oxygen-deficient States turned it into a huge crisis. This can be attributed to the haphazard system and red-tapism which held back timely deliveries.
- Laxity by States in setting up oxygen plants
- During the first wave of COVID-19 in 2020, the central government held discussions with the oxygen manufacturers’ association for the augmentation of oxygen capacity based on potential requirements.
- State governments were asked to set up oxygen plants at the bigger hospitals in their jurisdictions and funds were allocated to do so by January 2021. But by that time, the first wave was losing its ground and thus the urgency to set up oxygen plants was not paid attention to.
- While few States set up oxygen plants, most of the States did not proceed to set up the oxygen plants. This laxity on part of some States landed them in extreme difficulties during the second wave of the pandemic.
- Black-marketing – As the oxygen demand exponentially rose during the peak of the second wave of the COVID-19, the black-marketing of this essential medical supply began to plague the market creating a demand-supply mismatch. It also led to the exponential rise in the prices of oxygen cylinders which harmed the general public financially and added to their financial woes in the time of the pandemic.
- Oxygen rationing
- The oxygen rationing method is different for different countries. However, in India, the method mainly implies the central government collecting data on oxygen beds and ICU beds from all COVID-19 hospitals in each state and allocating a certain quantity of oxygen to the State, according to the amount that was deemed to be necessary for the treatment of every patient. In turn, each state allocates a quota to each district and each district to the hospitals under their jurisdiction.
- It also involves monitoring and controlling oxygen wastage.
- However, these methods turned out to be counterproductive during the second wave because the requirements of patients were not stable, ICU oxygen requirements were higher, vendors under-filled the oxygen cylinders sometimes intentionally, or due to lapses in the filling process and others.
What can be done to avoid the recurrence of such a crisis?
- Creation of oxygen storage capacities – One of the major problems that were encountered during the oxygen crisis was the problem in transport and storage of oxygen and the lack of cryogenic tankers. More of these tankers could be arranged. Hospitals can be asked to install, maintain, and operate their oxygen plants, strengthen liquid oxygen infrastructure when possible, and/or provide for standby oxygen concentrators and cylinders.
- Management of existing oxygen supply channels and proper communication of information about demand and supply – A lot of medical oxygen is wasted. It is said that oxygen plant professionals should be brought in to guide hospitals on how to best manage their supplies. Additionally, there should be a standardized flow of information on the demand and supply of oxygen at all levels.
- Setting up of PSA oxygen plants – PSA (Pressure Swing Adsorption) plants could be set up as these plants can draw oxygen directly from the air and can directly pipe the harvested gas into hospitals. These are long-term investments and cost-effective and ensure that hospitals always have a backup supply of oxygen.
- Minimizing red-tapism and setting up of clear governance arrangement protocols – To be prepared for such crises beforehand, there should be the development of standard operating procedures on buffer stock, the flow of information, and oxygen allocations. Such issues which hinder the free flow of oxygen from one place to another must be dealt with and government restrictions should be minimised.
- Top-down allocation and distribution of oxygen – There should be the flow of information upwards (demand) and downwards (allocation) so that each level gets its due allocation and no such crisis recurs
- Protection of newly built plants from failure – Proper care and management of newly built plants could help the hospitals to protect them from failure and meet the sudden demand for oxygen during crises. Regular functioning audits of the plants would also need to be conducted and capacity augmentation to be done as needed..
Government initiatives
- The central government launched “Project O2 For India” to ensure oxygen supply. The government is also building up the supply chain of critical materials and parts of oxygen plants. Funding for plants is being arranged through PM CARES as well as corporate sponsorships via CSR funding.
- Many States are also enhancing their capacities of oxygen storage and production.
- The production capacity is also being raised at national level.
- Proper flow of information and oxygen allocation is being done.
- The capacity of oxygen tankers and their number is being increased.
- Other initiatives include optimization of logistics, improvement of oxygen storage, and easing norms of procurement.
Conclusion
As the nation prepares itself to face the upcoming third wave of the pandemic, it is time that adequate measures are taken to avoid such a crisis. Hospitals also need to be assisted financially through cheap loans and other instruments to set up oxygen storage facilities and arrange tankers. A multi-pronged approach while involving all the stakeholders will be the way forward.
Practise Question
Q. Comment on the oxygen crisis in India during the second wave of the COVID-19 pandemic and suggest measures to prevent the recurrence of such a crisis.
- https://www.cgdev.org/blog/how-india-can-prevent-next-oxygen-shortage-crisis
- https://www.orfonline.org/research/preventing-a-repeat-of-the-covid-19-second-wave-oxygen-crisis-in-india/
- https://www.theglobalfund.org/en/blog/2021-05-26-the-pandemic-hurt-everyone-indias-oxygen-crisis-from-the-frontlines/
- https://www.indiatoday.in/india-today-insight/story/india-s-oxygen-crisis-what-needs-to-be-done-1800584-2021-05-09
- https://www.indiatoday.in/india-today-insight/story/india-s-oxygen-crisis-what-needs-to-be-done-1800584-2021-05-09

Nice